What Is Achilles Tendinopathy?
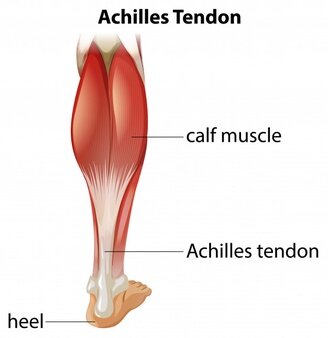
The Achilles tendon is a tendon shared by two major muscles of the calf: gastrocnemius and soleus. It inserts onto the calcaneus (heel-bone). The function of the Achilles tendon and its associated musculature is to raise the heel and lower the forefoot. The tendon allows for recoil and shock-absorbance in the foot during functional activities.9 It is the biggest and strongest tendon in the human body!
The Achilles tendon is susceptible to injury with overloading the tissue or repetitive use. Injuries can occur in both athletes and non-athletes. A more acute, inflammatory injury would be considered a tendinitis or a tear. However, chronic Achilles tendon issues are often categorized as Achilles Tendinopathy. This condition is degenerative in nature and is usually diagnosed in the absence of a tear or complete rupture. The evidence for these degenerative changes in the tendon have been studied in those undergoing surgery of the Achilles tendon. Examining the tissue, degenerative changes were observed in the tendon fiber’s structure. 11
Who Is At Risk?
Risk factors for Achilles tendinitis specifically include ankle stiffness, decreased plantarflexion strength (ability to push off or raise heel), increased foot pronation (flat foot arch) and visualized abnormal tendon structure on imaging. Medical conditions that increase risk for Achilles Tendinopathy include obesity, hypertension, hyperlipidemia, and diabetes.1
How Does Achilles Tendinopathy Develop?
Achilles tendinopathy can be a result of over-stressing the Achilles tendon itself with excessive sport activity. However, this condition can occur with every day activities such as walking. Achilles pain can seemingly come on suddenly or slowly over time. In this author’s experience, this population usually has a past history of injury, whether new or old, in the ankle/foot region, knee, hip and/or lumbar spine (A lot of options!).
Over time compensations develop during walking, causing increased stresses in the Achilles tendon. A good example of this would be someone who has had repeat ankle sprains that have resulted in stiffness in their ankle, requiring the Achilles tendon to compensate for these losses in ankle mobility. Those with chronic foot and ankle disorders likely have chronic motor control and movement impairments.6 It then becomes vital to correct these impairments to restore normal function.
How Do We Treat Achilles Tendinopathy?
Treatment for Achilles tendinopathy can include joint mobilizations, dry needling, stretching, and muscle re-education, all of which can be provided by a physical therapist.
Ankle Mobilizations and Stretching – Ankle dorsiflexion is commonly limited in this population, which is required for normal walking and running mechanics. Evidence has shown that mobilizing the ankle and stretching the calf musculature can improve ankle range of motion.4,5
Dry Needling – A systematic review analyzing the effects of dry needling to treat tendinopathy shows that there are improvements in patient reported outcomes of pain and function.8 Collagen is an important component of the architecture of the Achilles tendon tissue and is often degenerated in those with Achilles tendinopathy. One theory of dry needling’s mechanism of effect is that the mechanical pressure of the needle to the tendon triggers tissue remodeling.2
Soft Tissue Mobilizations – There is evidence for the use of soft tissue mobilizations in Achilles tendinitis.3 A soft tissue mobilization emphasizing massage beginning from the heel up toward the calf can help resolve swelling around the Achilles tendon if present.
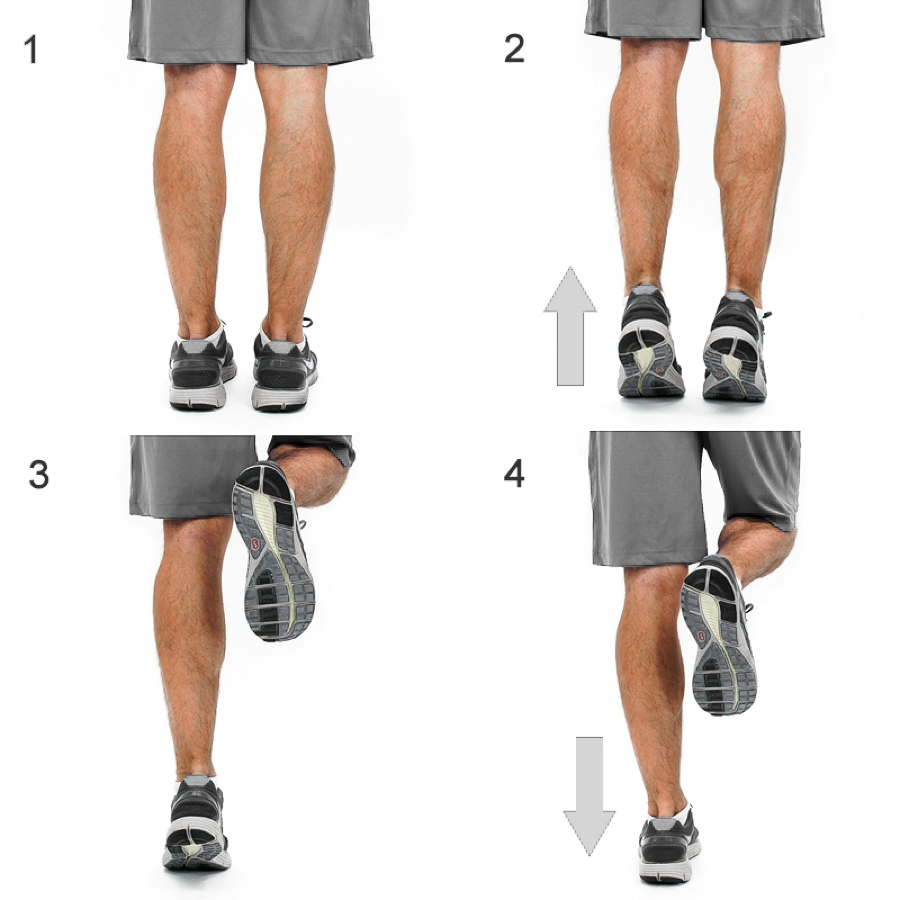
Muscle Re-Education – There is a significant amount of evidence supporting eccentric exercise as effective treatment of Achilles tendinitis in the chronic stage.7 Let’s step through an eccentric heel raise. Begin by raising both heels (standing on your toes) and then lift one foot off the ground. Then slowly lower the heel of the other foot to the ground. The benefits of eccentric exercise may be related to the concept of tissue time under tension in relation to increasing tissue reformation and strengthening.10 This is a great way to strengthen the Achilles tendon. Increasing the resiliency of the Achilles tendon with heel raise exercises appears to be a vital component of recovery.
Whether you are dealing with an inflamed, degenerated, torn or even ruptured tendon, a physical therapist can help diagnosis and differentiate these conditions.
If you would like to speak with a physical therapist please click below to schedule an evaluation or schedule a 20 minute FREE screen.
The WildHawk PT blog is for information purposes only. The bloggers are licensed physical therapists. The content published in this blog represents the opinion of the author based on their expertise and experience. The content provided does not constitute medical advice and should not be relied on for making personal health decisions.
References:
1. Carcia CR, Martin RL, Houck J, Wukich DK; Orthopaedic Section of the American Physical Therapy Association. Achilles pain, stiffness, and muscle power deficits: achilles tendinitis. J Orthop Sports Phys Ther. 2010;40(9):A1‐A26. doi:10.2519/jospt.2010.0305
2. Chen JT, Chung KC, Hou CR, Kuan TS, Chen SM, Hong CZ. Inhibitory effect of dry needling on the spontaneous electrical activity recorded from myofascial trigger spots of rabbit skeletal muscle. Am J Phys Med Rehabil 2001; 80: 729–35.
3. Christenson RE. Effectiveness of specific soft tissue mobilizations for the management of Achilles tendinosis: Single case study‐ Experimental design. Manual Therap. 2007;12;63‐71.
4. Hernández-Guillén D, Blasco JM. A Randomized Controlled Trial Assessing the Evolution of the Weight-Bearing Ankle Dorsiflexion Range of Motion Over 6 Sessions of Talus Mobilizations in Older Adults. Phys Ther. 2020 Apr 17;100(4):645-652. doi: 10.1093/ptj/pzaa003. PubMed PMID: 31944252.
5. Kang MH, Oh JS, Kwon OY, Weon JH, An DH, Yoo WG. Immediate combined effect of gastrocnemius stretching and sustained talocrural joint mobilization in individuals with limited ankle dorsiflexion: A randomized controlled trial. Man Ther. 2015 Dec;20(6):827-34. doi: 10.1016/j.math.2015.03.016. Epub 2015 Apr 2.
6. Kangas J, Dankaerts W, Staes F. New approach to the diagnosis and classification of chronic foot and ankle disorders: identifying motor control and movement impairments. Manual therapy 2011; 16(6): 522-30.
7. Kingma JJ, de Knikker R, Wittink HM, Takken T. Eccentric Overload Training in Patients with Chronic AT: A systematic review. Br J Sports Med. 2007;41(6):e3.
8. Krey D, Borchers J, McCamey K. Tendon needling for treatment of tendinopathy: A systematic review. Phys Sportsmed. 2015 Feb;43(1):80-6. doi:10.1080/00913847.2015.1004296. Epub 2015 Jan 22. Review.
9. Moore KL, Agur AMR, Dalley AF. Essential clinical anatomy. 4th ed. Baltimore: Lippincott Williams & Wilkins, 2011.
10. Skovdal Rathleff M, Thorborg K, Bandholm T. Concentric and eccentric time-under-tension during strengthening exercises: validity and reliability of stretch-sensor recordings from an elastic exercise-band. PLoS One. 2013;8(6):e68172. Published 2013 Jun 25. doi:10.1371/journal.pone.0068172
11. T E O Schubert, C. W. (2005). Achilles tendinosis is associated with sprouting of substance P positive nerve fibres. Ann Rheum Dis , 1083-1086.fckLR